Atherosclerosis and Arteriosclerosis

Atherosclerosis and Arteriosclerosis
Objectives
At the end of this PDF Notes, student will be able to
• Define Atherosclerosis
• Identify the risk factors for atherosclerosis
• Describe the symptoms of atherosclerosis
• Explain the pathogenesis of atherosclerosis
• Explain arteriosclerosis
• Difference between arteriosclerosis and atherosclerosis
• Describe the causes of it
• Briefly explain the risk factors
• Describe the treatment of it
Atherosclerosis
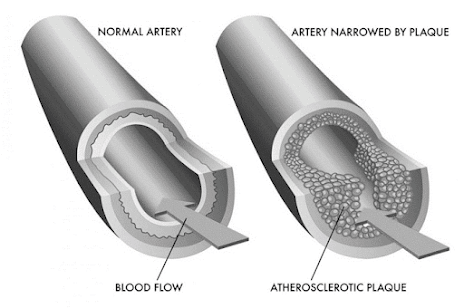
• Atherosclerosis or atheroma
• Patchy focal disease of arterial wall
• Patchy thickening of the intimal layer of arterial wall
• Due to lipid deposition or fibrosis tissue formation
Major risk factors of Atherosclerosis
• Age
• Family history & genetics
• Racial risk – whites are at greater risk than
blacks
• Excess lipid deposition
• Hypertension
• Smoking
• Diabetes mellitus
Minor risk factors of Atherosclerosis
• Obesity
• Lack of exercise
• Sedentary life style
• Use of oral contraceptives
• Alcohol consumption
• Stressful life
• Dietary factors
• Viral infection
Symptoms of Atherosclerosis
Symptoms vary depending on the organ involved
Heart
– Restricted blood supply to heart
– Angina & Myocardial infarction
– Shortness of breath
– Sweat
– Nausea
– Dizziness
– Palpitation
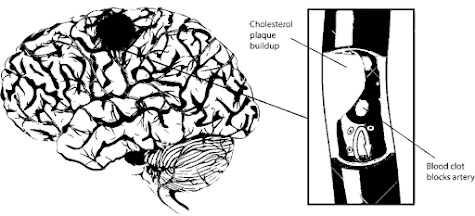
Brain
– Narrowing of arteries supplying brain
– Causes ischemic attacks
– Head ache
– Paralysis of one side of the body
– Numbness in various parts
– Visual disturbance
– Stroke
Abdomen
– Dull pain is felt in the abdomen
– Due to blockage of arteries supplying intestine
– Vomiting
– Diarrhoea
– Constipation
Leg
– Narrowing of artery supplying leg
– Pain in the leg
– Hair loss in leg
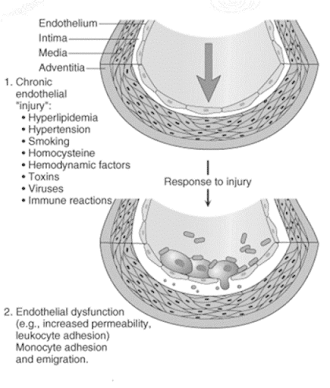
Pathogenesis of Atherosclerosis
Endothelial injury
• Atherosclerosis is initiated by injury of endothelium
• In large & medium size arteries
• Causes include smoking
• Hypertension
• Chronic hyperlipidemia
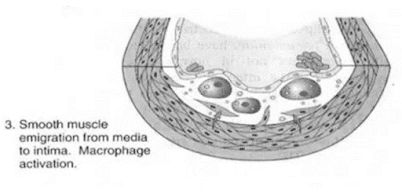
Internal smooth muscle cell proliferation
• Subsequent to endothelial injury
• Following disruption of endothelial layer
• Smooth muscle cell of blood vessels
• Cells of endothelium
• Proliferate under influence of – PGDF, EDGF, TGF β
• More synthesis of matrix protein
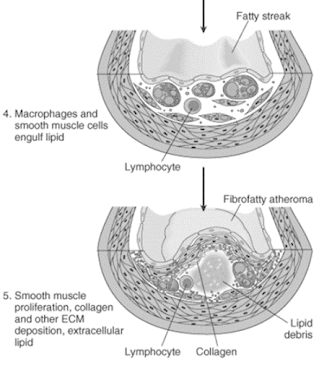
Lipoprotein entry into the intima
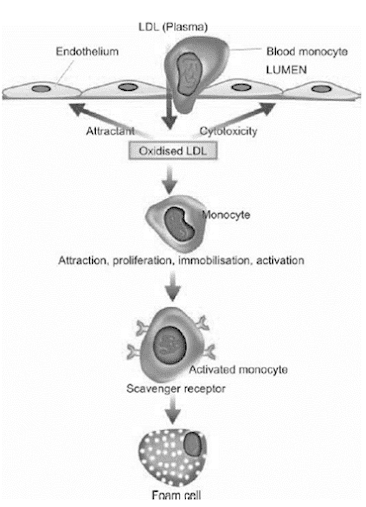
• LDL from blood enters intima & get oxidized
• Oxidized LDL attracts monocytes
• Activates monocytes to macrophages
• Combination of oxidized LDL & macrophages – Lipid laden foam cells
• Major factor contributing to plaque formation
Mechanisms involved in the formation of Foam cells
Summary
• Atherosclerosis or atheroma is a patchy focal disease of arterial wall
• Patchy thickening of the intimal layer of arterial wall due to lipid deposition or fibrosis tissue formation
• The main mechanism involved in the development of atheroma is endothelial injury
• Endothelial injury is followed by proliferation and formation of foam cells
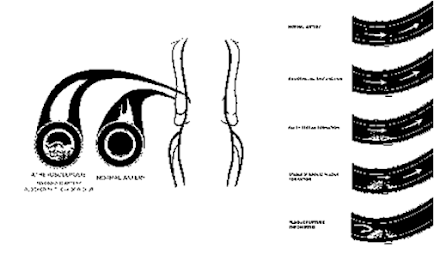
ARTERIOSCLEROSIS
• Arteriosclerosis refers to the thickening and hardening of the medium or large arteries.
• Atherosclerosis is a form of arteriosclerosis in which cholesterol deposits line the inner wall of the artery.
• Arteriosclerotic plaque is a build-up of calcium on the inside of the artery walls. Both terms tend to be used interchangeably to describe the clogging and hardening of the arteries.
• Arteriosclerosis occurs either as a result of high blood pressure, high cholesterol or both.
• High blood pressure can cause the arteries to become stiff and thick, which restricts blood flow throughout the body.
• High cholesterol can cause an excessive build-up of plaque inside the arteries that significantly restrict blood flow.
• Arteriosclerosis most commonly occurs in the arteries of the heart, but it can affect any arteries within the body.
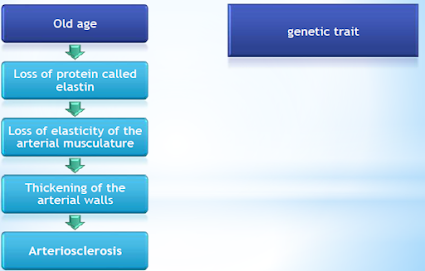
Factors that cause arteriosclerosis
Risk factors of Arteriosclerosis
• obesity
• smoking
• diabetes
• Inactivity
• diet high in saturated fat & low in healthy fruits, vegetables
Treatment of Arteriosclerosis
• Lifestyle Modifications-In the early stages of arteriosclerosis, lifestyle modifications include eating a diet low in cholesterol and salt.
• A healthy diet, along with getting regular exercise, might help slow and possibly even stop the progression of the disease.
• smokers should stop in order to prevent further artery damage.
• Medications– Medications, including those for blood pressure and high cholesterol, may be used to control conditions that have contributed to the development of arteriosclerosis.
• aspirin and anticoagulants
• Bypass Surgery– using a blood vessel from another part of the body or a synthetic tube to completely bypass the damaged artery.
Signs of Arteriosclerosis
• A decreased pulse in a narrowed artery
• Decreased blood pressure in a limb
• A bulge in the abdomen or behind the knee
• High blood pressure
• Kidney infection
• Shortness of breath
• Dizziness
• Neurological Symptom-Arteriosclerosis may affect the arteries that supply the brain.
Summary
• Arteriosclerosis refers to the thickening and hardening of the medium or large arteries
• artery walls become calcified or hardened which results in a loss of flexibility and elasticity
• Arteriosclerosis is a disease process that occurs gradually over time, and although the hardening of the heart’s arteries receives most attention, arteriosclerosis can happen anywhere along the miles of these blood vessels in your body
• Avoid smoking as this can increase the risk of complications such as stroke and heart attack
FAQs
1. Is arteriosclerosis the same as atherosclerosis?
No, arteriosclerosis is a broader term that includes atherosclerosis as one of its types. Arteriosclerosis refers to the hardening and thickening of arteries, while atherosclerosis specifically involves plaque buildup.
2. What role does genetics play in atherosclerosis?
Genetics can influence how your body processes fats and cholesterol, impacting your risk of atherosclerosis. If you have a family history of the condition, you may be more susceptible.
3. Can atherosclerosis be reversed?
Atherosclerosis can be managed and its progression slowed through lifestyle changes, medications, and medical procedures. However, it is typically not fully reversible.
4. What are the long-term complications of atherosclerosis?
Long-term complications may include heart disease, stroke, peripheral artery disease, and kidney problems.
5. How can I reduce my risk of atherosclerosis?
You can reduce your risk by maintaining a healthy lifestyle, including a balanced diet, regular exercise, not smoking, and managing conditions like diabetes and high blood pressure. Regular check-ups with your healthcare provider are essential for early detection and prevention.
6. What are the primary treatment options for atherosclerosis?
The treatment of atherosclerosis typically involves lifestyle changes, such as a heart-healthy diet, regular exercise, and smoking cessation. Medications, such as statins, antiplatelet drugs, and blood pressure medications, may also be prescribed. In some cases, medical procedures like angioplasty or bypass surgery are necessary.
7. Can atherosclerosis lead to heart attacks and strokes?
Yes, atherosclerosis is a leading cause of heart attacks and strokes. When the plaque in the arteries ruptures, it can trigger blood clots that block blood flow to the heart or brain, resulting in these life-threatening events.
8. Is atherosclerosis preventable?
While certain risk factors like age and genetics are beyond your control, many aspects of atherosclerosis are preventable. By adopting a healthy lifestyle, managing your weight, eating a balanced diet, and controlling conditions like hypertension and diabetes, you can significantly reduce your risk.
9. How is atherosclerosis diagnosed?
Atherosclerosis is diagnosed through various tests, including cholesterol blood tests, ultrasound, angiography, and coronary calcium scans. Your healthcare provider will assess your risk factors and recommend the most appropriate diagnostic tests.
10. What are the dietary recommendations for preventing atherosclerosis?
To prevent atherosclerosis, it’s essential to maintain a heart-healthy diet. This includes reducing saturated and trans fats, increasing fiber intake, and consuming more fruits, vegetables, and whole grains. It’s also crucial to limit salt and sugar intake and watch portion sizes to maintain a healthy weight.




1 thought on “Atherosclerosis and arteriosclerosis – B. Pharma 2nd Semester Pathophysiology notes pdf”