Aminoglycosides
Contents
• Introduction
• Chemistry of Aminoglycosides
• Structure and Activity Relationship of Aminoglycosides
• Spectrum of activity of Aminoglycosides
• Uses of single Aminoglycosides / combinations
• Mechanism of Action of Aminoglycosides
• Study of Individual compounds
Learning
Objectives
At the end of this
lecture, student will be able to
• Understand the chemistry of Aminoglycosides
• Explain the SAR of Aminoglycosides
• Discuss the spectrum of activity of Aminoglycosides
• Explain the general mode of action of Aminoglycosides
• Discuss the structures and specific uses of individual
Aminoglycosides
• Streptomycin 1st aminoglycoside antibiotic used in
chemotherapy.
• Other compounds closely related in structure are Kanamycin,
Neomycin, Paramomycin, Gentamycin, Tobramycin, Netilmycin and Amikacin (semi
synthetic derivative of Kanamycin A)
• All aminoglycoside antibiotics are absorbed very poorly
following oral administration yet some of them eg. Kanamycin, Neomycin and paramomycin
are administered orally for the treatment of G.I. Infections.
• Due to their broad spectrum anti-microbial activity, they
are used to treat systemic infections (parenteral route).
• Side effects include ototoxicity and nephrotoxicity- this
has restricted their systemic use to serious infections or to treat infections
caused bacterial strains resistant to other agents
Aminoglycosides
Chemistry
• Amino-glycosides are amino-sugars linked glycosidically.
• All have at least one aminohexose, or a pentose lacking an
amino group eg. Streptomycin, neomycin and paromomycin.
• They contain a highly substituted 1, 3-diaminocyclohexane
central ring eg. Kanamycin, neomycin, gentamycin
• They are strongly basic compounds that exist as
polycations at physiological pH.
• Their inorganic salts are highly water soluble
• They are available as sulphate salts
• They distribute well into most body fluids but not CNS,
bone or fatty connective tissue
• They are concentrated in the kidneys, and excreted by
glomerular filtration
• They are not metabolized in vivo
Mechanism
of action
• They act directly on the bacterial ribosome to inhibit the
initiation of protein synthesis and to interfere with the translation of the
genetic messages.
• They bind to the 30S ribosomal subunit to form a complex
that cannot initiate proper aminoacid polymerization
• This binding to ribosomes also causes misreading mutations
of the genetic code, due to the failure of specific aminoacyl RNA’s to
recognize the proper codons on mRNA and hence cause incorporation of improper
aminoacids into the peptide chain.
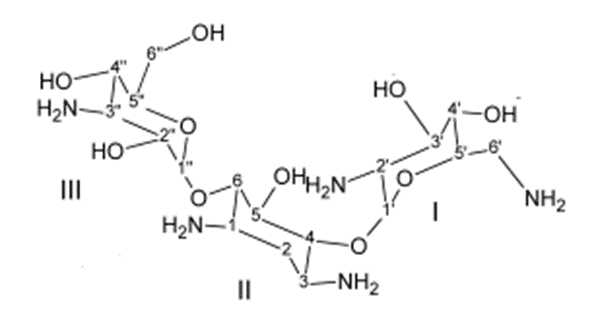
SAR
Ring I:-
• Crucially important for characteristic broad spectrum
anti-bacterial activity and it is the primary target for bacterial inactivating
enzymes.
• Amino functions at 6’ and 2’ are important as Kanamycin –
B (6’-amino -2’amino) is more active than Kanamycin – A (6’- Amino- 2’-
hydroxyl) which in turn is more active than Kanamycin – C (6’-
hydroxyl-2’-amino group)
• Methylation at either the 6’-carbon or 6’-amino positions
does not lower anti-bacterial activity, but confers resistance to enzymatic
acetylation of the 6’-amino group.
• Removal of the 3’-hydroxyl or the 4’-hydroxyl or both in
the Kanamycins (eg., 3’,4’-dideoxy kanamycin B or dibekacin) does not
Ring- II:-
• Few modifications of ring II functional groups is possible
without appreciable loss of activity.
• 1-amino group of Kanamycin –A, can be acylated eg.
Amikicin and the activity is largely retained.
• Netilmicin retains the antibacterial potency of sisomicin
and is resistant to several additional bacteria-inactivating enzymes.
Ring III
• Ring III functional groups are less sensitive to
structural changes than those of either Ring I and II
• 2”–deoxy derivatives are less active than their
2”–hydroxyl counterparts (eg. 2”–deoxy gentamycin).
• 2” – amino derivatives (eg. Seldomycins) are highly
active.
• The 3”
– amino group
of Gentamycins may
be 1° or
2° with high antibacterial potency.
• The 4”-hydroxyl
group maybe axial
or equatorial with
little change in potency
Spectrum of
Activity
• Aminoglycosides are classified as broad – spectrum
antibiotics, but they are mostly used in the treatment of serious infections
caused by aerobic Gram -ve bacilli. – Aerobic Gram-ve and Gram+ve cocci
(exception – staphylococci) are less sensitive. So in these infections β-lactam
and other antibiotics are preferred.
• Aminoglycosides
and β-lactam antibiotics
exert synergetic effect against some bacterial strains-
damage to the cell well is believed to increase the penetration of the aminoglycosides
into the bacterial cell
• However the two antibiotic types should not be combined in
the same solution as they are chemically incompatible
|
DRUG/DRUG COMBINATION |
USE |
|
Streptomycin |
In the chemotherapy of tuberculosis, brucellosis, tularemia and |
|
Paramomycin |
Chemotherapy of amoebic dysentery |
|
Carbenicillin + Gentamycin |
Synergistic against Gentamycin- sensitive strains of P-aeruginosa and |
|
Penicillin G + Streptomycin or |
In the treatment of enterococcal endocarditis |
Damage of the cell wall caused by the β-lactam antibiotic
will increase penetration of aminoglycoside into the bacterial cell wall.
Infections:
• Brucellosis –
Undulant fever, an intermittent fever caused by organisms (Brucella-bacteria,
primarily pathogenic in animals but which may affect man) transmitted in infected
milk from cattle and goats.
• Tularemia – An
undulant fever (caused by Brucella tularensis) may be infected to man by
various insects or by rats. The lymph glands are involved and they may
suppurate.
• Bubonic Plague –
An acute fever endemic in Asia and Africa. Causative organism – Pasteurella
pestis transmitted by the bites of fleas that have derived the infection from
diseased rats. (Characterized by buboes)
• Glanders – A
contagious disease of horses and asses sometimes communicated to man through a
crack in the skin.
• Streptomycin is equally effective in inhibiting initiation
and causing misreading.
• Spectinomycin prevents the initiation of protein synthesis
but does not cause misreading.
• All are bactericidal except Spectinomycin.
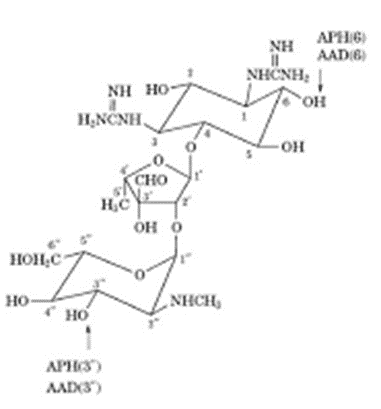
Streptomycin
• The organism that produce streptomycin, streptomyces
griseus, also produce other antibiotic compounds– hydroxyl-streptomycin,
mannisido-streptomycin and cycloheximide
• Streptomycin is referred to as streptomycin – A and
mannisido
• The problem with the use of streptomycin is the early
development of resistant strains of bacteria necessitating a change in therapy.
• Other problems are chronic toxicities:-
• Neurotoxic reactions include vertigo, disturbance of
equilibrium, diminished auditory perception
• Nephrotoxicity.
• Neomycin (sulfate) [MYCIFRADIN, NEOBIOTIC]
• Kanamycin
• Isolated from
• Streptomyces Kanamycelicus
KANAMYCIN:
Uses:
• In the treatment of infections of the intestinal tract
(eg., bacillary dysentery)
• In the treatment of systemic infections from Gram –Ve
bacilli (eg., Klebsiella, Proteus, Enterobacter and Serratia spp.)
• Also used for pre-operative antisepsis of the bowel.
Gentamycin:
(Sulfate)
• It has a broad spectrum of activity against many common pathogens
both gram +Ve and gram -Ve
Uses:-
• It is effective in the treatment of a variety of skin
infections especially in the treatment of burns complicated by pseudomonemia.
• Used for serious systemic and genitourinary tract
infections caused by gram –Ve bacteria particularly Pseudomonas, Enterobacter
and Serratia spp.